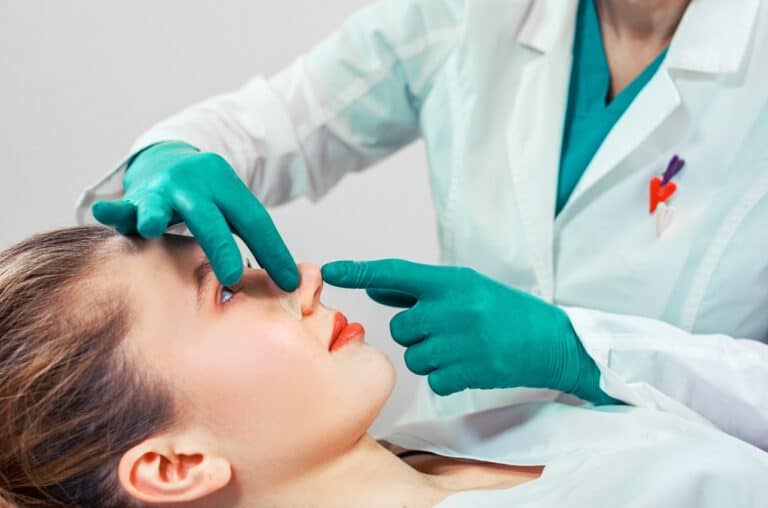
Many individuals approach rhinoplasty with questions and uncertainties, especially when it comes to insurance coverage. At the Rhinoplasty Center of Long Island, we regularly help patients clarify what their policies do and do not cover.
Your reasons for seeking nasal surgery can significantly influence whether your insurance will assist with costs. Understanding these details helps you make informed decisions and avoid unexpected expenses. Let us guide you through the essentials of insurance and rhinoplasty so you can confidently plan your next steps.
Key Takeaways
- Medical Necessity Matters: Insurance often covers rhinoplasty only when it addresses medical issues, such as breathing problems or trauma.
- Cosmetic Procedures Rarely Qualify: Purely cosmetic rhinoplasty is almost never covered by insurance companies.
- Documentation Is Crucial: Detailed physician notes and medical records are required for insurance approval.
- Preauthorization Is Essential: Most policies require approval from your insurer before surgery to confirm coverage.
- Combined Surgery May Be Possible: Some patients qualify for partial coverage if both functional and cosmetic issues are present.
- Out-of-Pocket Costs Vary: Be prepared for potential self-pay expenses, even with insurance involvement.
- Consulting Professionals Helps: Meeting with our team can clarify your specific situation and provide guidance tailored to your needs.
Understanding Rhinoplasty: Surgery Overview and Common Objectives
Rhinoplasty, often known as a “nose job,” is a surgical procedure that reshapes or repairs the nose. People choose rhinoplasty for a wide range of reasons. Some undergo surgery for cosmetic refinements, while others seek it for functional or health-related motives.
For many, this surgery addresses breathing difficulties caused by a deviated septum or nasal obstruction. Others aim to repair an injury after trauma or resolve congenital abnormalities. Cosmetic rhinoplasty, in contrast, adjusts the appearance of the nose without correcting medical issues.
With awareness of these common objectives, you can better understand if your personal goals align with medical necessity standards required by insurance providers.
Medical vs. Cosmetic Rhinoplasty
Medical rhinoplasty focuses on functional improvements, like restoring airways or correcting birth defects. Cosmetic rhinoplasty deals strictly with appearance, such as reshaping the nose or refining the tip.
If your interest is purely aesthetic, insurance will almost certainly not contribute financially. If you have breathing problems or nasal trauma, there may be a greater chance for at least partial coverage.
Common Reasons People Choose Rhinoplasty
These motivations include a desire for enhanced facial balance, correcting structural defects, or improving nasal function. Injuries, hereditary conditions, and long-standing breathing difficulties all play a role in driving patient interest.
Taking time to clarify your own reasons for considering rhinoplasty will be the first step in determining insurance eligibility.

When Does Insurance Cover Rhinoplasty?
Insurance coverage depends greatly on whether the surgery is deemed medically necessary. This section outlines the main conditions under which coverage might apply.
Situations Where Insurance Often Provides Coverage
Patients typically seek insurance approval for rhinoplasty when they face medical challenges. Coverage is more likely if you experience the following:
- Documented Breathing Problems: Chronic obstruction or inability to breathe normally through the nose may qualify as a medical necessity.
- Septoplasty Requiring Structural Repair: Surgeries that correct a deviated septum are often covered if conservative treatments have failed.
- Reconstructive Needs After Trauma: If your nose has suffered significant damage from injury or accident, insurance may approve reconstructive rhinoplasty.
- Congenital Deformities: Procedures that correct birth defects, such as cleft palate or other nasal deformities, may receive insurance support.
- Previous Surgical Complications: Corrections for significant breathing impairment caused by a prior surgery can sometimes be covered.
Insurance companies typically require documented evidence confirming one or more of these situations. If your surgery falls into any of these categories, your likelihood of receiving coverage increases.
Cosmetic-Only Rhinoplasty and Insurance
If your goal is to change the appearance of your nose without a medical issue, insurance does not provide reimbursement. Purely aesthetic procedures fall outside company guidelines.
Many patients with combined concerns, for example, breathing issues coupled with a desire for cosmetic change, ask about partial coverage, which we will address later in this article.
The Importance of “Medical Necessity”
Insurance companies rely on strict definitions of what qualifies as medically necessary. This label means the surgery is required to treat a medical condition and not simply for cosmetic enhancement. Each insurance provider may have its own criteria and policies for determining medical necessity.
A thorough medical evaluation and clear physician documentation are vital for meeting these requirements.
How Insurance Determines Coverage: The Approval Process
Our team finds that the insurance process can be confusing for many patients. To help you move forward with greater confidence, here is a detailed breakdown of how coverage decisions are typically made.
The Role of Documentation
The approval process revolves around comprehensive medical documentation. You must provide clear evidence outlining the health problem that surgery will address. This often means a diagnostic workup, physician’s notes, CT scans, and records of previous treatments.
Preauthorization Requirements
Most insurance policies require preauthorization before you undergo surgery. Preauthorization is a review performed by your insurer to ensure the procedure meets their criteria for medical necessity.
You, your surgeon, or a specialist must submit supporting documents and clinical notes describing your diagnosis and planned surgical intervention. Without preauthorization, insurance may deny coverage even if your condition seems to qualify.
Step-by-Step Overview of the Insurance Approval Process
It’s helpful to know the general steps that occur when seeking insurance coverage for rhinoplasty. Here is how the process usually unfolds:
- Initial Evaluation: The process begins when your surgeon examines you and determines that a functional problem exists.
- Testing and Imaging: You may undergo imaging or endoscopic exams to document your diagnosis.
- Documentation Compilation: Your surgeon will create a comprehensive record of the findings, often including photographs and descriptions of airway obstruction.
- Submission to Insurance: Our team submits all required paperwork for preauthorization review.
- Insurance Determination: The insurance provider reviews the file and issues an approval, denial, or request for further information.
- Appeals (If Needed): If your initial request is denied, an appeal with additional documentation may sometimes reverse the decision.
Knowing and following these steps can help you minimize unnecessary delays or administrative issues. Working with an experienced surgical practice like ours can make this process much smoother.
Types of Costs: What Insurance May Cover (and What It Will Not)
Breaking down the components of rhinoplasty expenses helps clarify what may be covered by insurance and what you might be responsible for paying.
Covered Versus Non-Covered Costs
When insurance covers a medically necessary rhinoplasty, it may pay for elements such as:
- Surgeon’s Fees for Functional Correction: Insurance typically covers fees associated with the portion of surgery treating the medical issue.
- Anesthesia and Facility Fees: Necessary anesthesia and hospital or surgical center costs can be included in the coverage.
- Follow-up Appointments Related to Medical Need: Visits to monitor healing and airway function after a functional procedure may qualify.
However, there are expenses that insurance almost never covers, including:
- Cosmetic Surgeon’s Fees: If any part of the procedure refines nasal appearance for nonfunctional reasons, you assume these costs.
- Additional Cosmetic Fees: Items such as implants or grafts used strictly for cosmetic improvement remain your financial responsibility.
- Optional Extras: Post-surgical treatments or enhancements that are not medically necessary are not included in standard coverage.
Knowing these distinctions helps you understand where personal expenses might arise after insurance support is factored in.
Combined Functional and Cosmetic Requests
Patients with both functional issues and cosmetic desires often wonder if they can address both needs under one surgery. At many practices, including ours, it is possible to combine the procedures.
In such combined cases, insurance only covers the aspects related to restoring health and function. You are still responsible for additional costs related to aesthetic changes.
Out-of-Pocket Costs and Payment Considerations
You should always be prepared for some out-of-pocket expenses even if you have been granted insurance coverage. Deductibles, copays, or costs related exclusively to aesthetic components all add up.
Speaking openly with your surgical practice’s billing and insurance team can provide a realistic estimate before surgery. This clarity helps avoid surprise bills and ensures you can make an informed decision.
What to Expect: The Patient Experience with Insurance and Rhinoplasty
Patients often feel concerned about navigating insurance processes on top of planning for surgery. Knowing what to expect can help you feel more empowered and prepared for the journey.
Typical Insurance Challenges and How to Handle Them
The insurance process is not always straightforward. We have identified certain common challenges patients encounter when seeking rhinoplasty coverage. Here are some you may wish to prepare for:
- Delays Due to Missing Documents: Make sure you gather and submit all required medical records early to avoid setbacks.
- Denials Based on “Insufficient Medical Necessity”: Some insurers may initially reject coverage, especially if documentation is unclear or incomplete.
- Confusion Over Combined Procedures: When both functional and cosmetic goals are addressed, it is important to separate costs and financial responsibilities from the beginning.
- Preauthorization Deadlines: Missing insurer deadlines for preapproval can result in denial of coverage.
Staying organized and communicating regularly with both your insurance provider and the surgical office can help prevent these issues from derailing your rhinoplasty plans.
Tips to Improve Your Chances of Insurance Coverage
At the Rhinoplasty Center of Long Island, we advise patients to:
- Keep all related medical appointments and records together in a dedicated folder.
- Follow your provider’s recommended non-surgical treatments, as these show conservative therapies were attempted first.
- Request an itemized financial estimate for both the medical and cosmetic aspects ahead of surgery.
- Do not hesitate to contact your insurer directly if you have questions about coverage or documentation requirements.
With these strategies, you stand the best chance of having your insurance help with rhinoplasty costs if you qualify.
Frequently Asked Questions About Rhinoplasty and Insurance
Patients commonly ask several questions during their rhinoplasty consultations regarding insurance. Let’s review the most frequent ones.
Will Insurance Cover a “Nose Job” for a Deviated Septum?
If you have documented breathing problems related to a deviated septum, medical rhinoplasty (also called septoplasty) often qualifies for coverage. You must demonstrate failed conservative management before insurance approval is granted.
Can I Combine Cosmetic Rhinoplasty With Medical Correction?
Combining procedures is common. Insurance will cover the medically necessary correction only, while cosmetic improvements are self-pay. Our surgeon can guide you through the financial breakdown.
What About Revision Rhinoplasty After a Prior Surgery?
If a previous nasal procedure resulted in documented breathing impairment or structural collapse, revision surgery may be covered. Thorough records and evidence of new symptoms are essential.
How Long Does Insurance Approval Take?
This varies widely by provider. After all documents have been submitted, preauthorization may occur within days or require several weeks. Starting the insurance process early in your planning phase reduces delays.
What to Do Next: Steps for Patients Considering Rhinoplasty
If you are thinking about rhinoplasty and want to understand your coverage options, taking the right first steps can make the process smoother. Here is a helpful overview to guide you.
Steps to Take If You Are Considering Insurance for Rhinoplasty
Before you begin, it is important to be well-prepared and informed. We suggest the following approach:
- Consult With a Board-Certified Surgeon: Your first step should be a complete exam and consultation, ideally with a specialist in both functional and cosmetic nasal surgery.
- Gather Your Medical Records: Collect any documentation regarding breathing problems, previous treatments, or accident reports.
- Check Your Insurance Policy: Read the fine print and speak directly to your insurer to clarify what is considered “medically necessary.”
- Request a Detailed Letter of Medical Necessity: Your surgeon will need to provide a comprehensive letter outlining why the procedure is required for your health.
- Obtain a Cost Estimate: Get a clear estimate outlining what insurance may pay versus what your responsibility will be, particularly if combining procedures.
A proactive, informed approach helps avoid unnecessary delays and confusion as you move forward with rhinoplasty planning.
The Value of Choosing an Experienced Practice
Selecting a practice with extensive experience in both surgical treatment and insurance coordination makes a significant difference. An experienced team will anticipate documentation needs, communicate clearly with your insurance carrier, and help ensure that your clinical information meets payer requirements.
At the Rhinoplasty Center of Long Island, we take pride in guiding patients from their first consultation through to post-surgical follow-ups. This comprehensive support can help you achieve the healthiest and most satisfying result possible, whether insurance participates or not.
Your Next Steps
Understanding whether insurance will cover your rhinoplasty can feel overwhelming, but with clear guidance, you are in a much stronger position. Insurance will typically support only the medically necessary components of nasal surgery. Purely cosmetic changes fall on the patient to finance personally.
Careful documentation, timely preauthorization, and clear communication between your surgical team and insurer form the cornerstone of a successful rhinoplasty experience. We encourage you to use this information as a starting point for your own decision-making process.
If you are considering rhinoplasty for medical or combined reasons, the Rhinoplasty Center of Long Island welcomes you to schedule a consultation. Our team stands ready to review your case, explore your insurance options, and help you understand the financial aspects, so you can move forward confidently toward your goals. Reach out today, and let’s take the next step together.